And what happens is that in some women, actually about 10% of women, there are bits of your endometrium—so bits of this lining of the womb—that are not in the endometrium anymore, but are actually growing and scarring tissues outside, a lot of the time within your abdominal cavity. So that can be on ligaments, on the intestine, on the bladder.
Solving endometriosis
Cyclana Bio
Endometriosis is a hidden disease affecting women with an invasive nature similar only to cancer. Having a win in endometriosis could massively propel our understanding in women's health.
- Endometriosis is a strange, invasive condition affecting 10% of women where the uterine lining grows outside the womb, causing severe pain and organ dysfunction.
- The disease remains "hidden" because its causes are poorly understood and symptoms are frequently dismissed, leading to an average diagnostic delay of 7 to 10 years.
- Current treatments are limited to invasive surgery or hormonal blockades that only suppress symptoms rather than reversing the disease.
- Innovation at Cyclana focuses on the "extracellular matrix"— the structure made of collagen and elastin—as a causal driver of the disease's inflammation and scarring.
Endometriosis
Endometriosis, which is often described as a hidden disease, is a very strange one because what happens is that your endometrium—the lining of your womb or your uterus—gets built up on a cyclical basis, on a monthly basis.
And they cause a lot of problems. They cause a lot of pain when that happens, but they also can cause really severe issues when they start getting into organs and disturbing how these organs work.
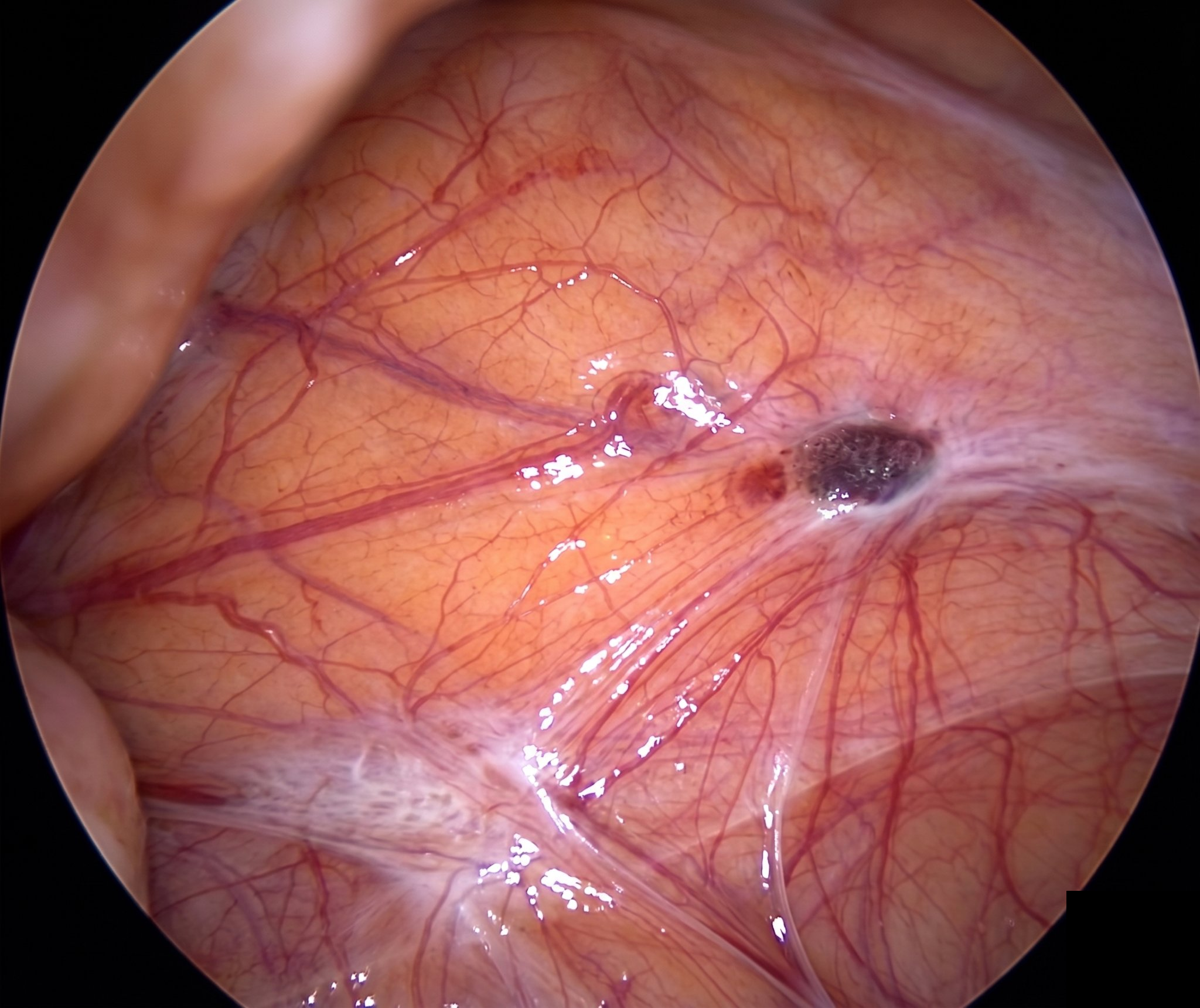
Peritoneal endometriosis lesion through the laparoscope; © Léa Wenger
We don't really understand how they get there, why they get there, and in whom. But yes, it's a condition that is very strange because it's these invading cells that aren't cancer, which is probably the only other disease I can think of that has this kind of invasive nature.
So it's a hidden disease, partly because the true causes and drivers are already hidden. It's something that we kind of discover—we don't really observe it happening. But also because a lot of women don't necessarily know, or aren't listened to when they present with symptoms.
The average diagnostic time can range from 7 to 10 years in most cases, from the time a woman first has symptoms of endometriosis to the time where she finally gets a diagnosis. So it's hidden because for a long time in a woman's life, she might suffer from this disease without necessarily having an explanation for that suffering.
And it takes a very long time for them to eventually get believed—that this pain is something that isn't normal and that something is wrong.
Deep pain
Pain in the disease is a very important concept, even from a purely clinical perspective. That is the main thing we measure as an outcome currently in clinical trials to see whether a drug has worked.
It's an incredibly important aspect of the disease that is still slightly poorly understood, because we still don't know how much of the pain is coming from the direct lesions, how much is coming from broader inflammation in the body, and how much might be coming from the uterus itself.
Endometriosis is a disease that is thought to affect 1 in 10 women, so a huge number of people, but also one that affects them quite differently.

© Shutterstock
Some people might have what's called a superficial disease, where they might be in very excruciating pain at certain points in the month, then be all right for the rest of the month, and not necessarily have deep invasion into organs.
Whereas other women will have lesions that progress very deep and can cause gastrointestinal symptoms, gut symptoms, or bladder symptoms.
So as we're building this platform, we really want to understand this diversity in women—who should be treated by which treatments.
So few solutions
When we work with patients, when we work with people who volunteer to donate their menstrual fluid, for example, we do feel that there has been this whole life cycle or history of the disease. And for some women, that can be very tough, and there are very emotional conversations.
These women haven't necessarily been heard or listened to, and might have been looking for decades for treatments to take away this chronic pain.
And actually, we do talk to a lot of partners of women who have endometriosis, who are very involved with the disease and with the symptoms of their partner, and are there on certain days running in with a hot water bottle and a blanket and trying to help in whatever way they can.

© Wikimedia
But we also experience that a lot of the time they feel helpless, because there are so few solutions. We speak to a lot of people who say, "my wife has this condition, I don't know what to do, there's nothing that we can do, there's nothing that helps."
And even just being aware—spreading awareness to colleagues, especially male colleagues—anything that can spread understanding of how crippling this disease can be is good. The more awareness we have more broadly about the disease, the more chances we have to really tackle it together.
How is it currently diagnosed?
Definitive diagnosis is through laparoscopy. That means that the lesions that I mentioned, which are elsewhere in the body, are identified through surgery under general anaesthetic. The surgeon will remove them from the body and then send them to a pathologist, who will check whether they are indeed endometrial tissue. So the definitive diagnosis is a surgical one, which is quite invasive.
At the moment, treatment is mostly in two main ways: surgery to remove lesions, and hormonal blockade.
© Shutterstock
Surgery can work in some scenarios—for instance, if you have a lesion sitting on a nerve or burrowing into your intestine, then this operation can truly alleviate symptoms. But many women have this surgery and within 3 to 6 months all of the pain comes back, so it is not necessarily a solution for all.
The other aspect is hormonal blockade—things like progesterone-based contraceptive pills that block your cycles. Because it's a cyclical disease, if you block cycles, many women might not experience as many symptoms.
The problem is that about 30% of women are refractory to that treatment. Many women can't take hormones because of family history, for instance breast cancer, and for many it doesn't alleviate all the symptoms.
And you still get to the big problem of pregnancy. If you're taking contraceptive hormones, you are suppressing the symptoms rather than treating the disease. So we don't really have therapies that can truly address and reverse the disease itself.
Looking at the disease in a different way
So how do we disrupt this vicious cycle—no drugs being developed, people not looking into it because it's a hard disease, because no drugs have been developed?
I think it takes a lot of bold approaches and a lot of shots on target to see if we can find something that is actually going to reverse the disease.
And that's where we are making a bold attempt at Cyclana: we are really trying to look beyond hormones, beyond hormonal interventions, and beyond what exists in the current data, and say—let's try to build a whole platform that might look at the disease in a different way.
For us, that means looking at the disease not just as driven by cells, but as a disease driven by the extracellular matrix.
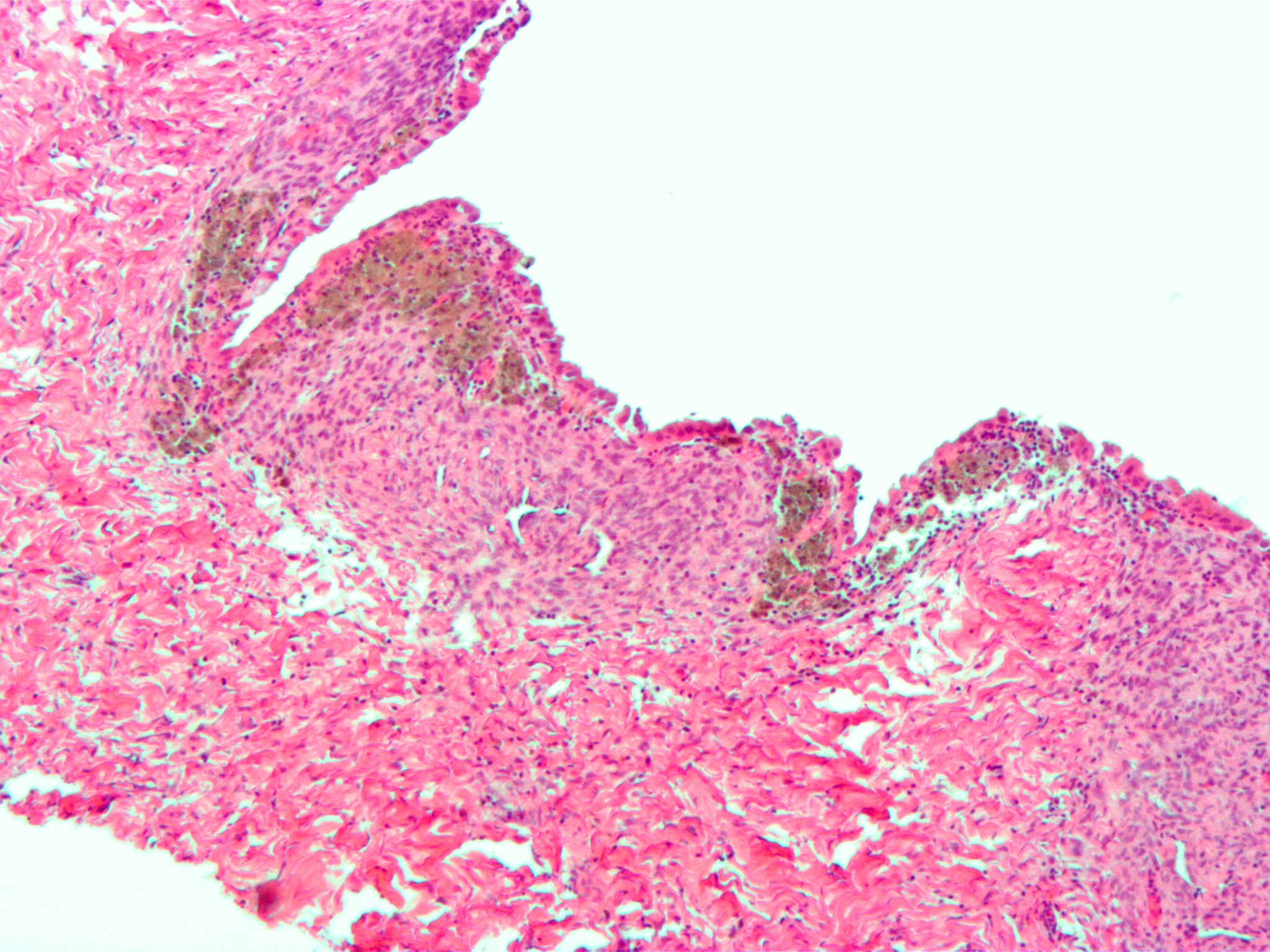
© Wikimedia
The extracellular matrix is what cells evolve in—things like collagen and elastin that give structure to the body. And that does go wrong in endometriosis. There is evidence that it is dysregulated.
So we want to bring these two aspects together: if you put diseased cells into a diseased matrix, can we start understanding where the causal or driving factors might be?
When we started looking into the matrix, we saw that it wasn't just a scaffold or structure for cells—it actually hugely influences how a cell behaves.
You can try to target an inflammatory pathway in the cell, but if you don't address the matrix driving that inflammation, as soon as you remove the treatment, it comes back.
So it is really an integral part of how tissues function and communicate, and something we haven't looked into enough to understand disease.
And even beyond endometriosis, a lot of what we're looking at is how one system invades another, and how that causes inflammation and scarring. These are very basic concepts that go beyond reproductive organs and should be expanded further.
Unlocking women's health
Better understanding endometriosis—having a win in endometriosis—could massively propel our understanding of women's health and health more broadly.
Because unlocking endometriosis means understanding how a cyclical symptomatic disease that happens in so many women can actually be reversed. That means understanding how it happens, and therefore shedding light more broadly on reproductive health and its association with infertility.
For instance, 40% of women with endometriosis are thought to suffer from infertility.
But beyond that, can it tell us more about the body as a whole?
© Wikimedia
There is also a financial argument. This is a disease that has lacked innovation, as is the case for many women's health conditions. Funding cycles self-perpetuate: if drugs fail and no breakthrough happens, people become hesitant to try again.
So there is a lot in the science that we can learn from endometriosis, but also a whole ecosystem change that could happen if we crack such a big disease.
Speaking to pharmaceutical companies, they also express that a win in endometriosis could signal that women's health is tractable—that we can understand it, that it's not too complicated, and that we should go after it.
Breaking a taboo
The social dimension of this condition is evolving, but still not present enough in general awareness. There has been huge progress. The fact that we can approach people and say, "here's a menstrual cup, can you donate your menstrual fluid?"—that reflects a lifting of taboos.
Talking about menstruation, public figures and celebrities have helped drive that movement, which has been very important for us to reach people.
But there are still many women and men who do not recognize these symptoms as symptoms.

© Shutterstock
It's a disease that is more than just pain. It can progress and become quite severe in some cases. So it's about understanding what the right treatment is for each individual, because not everyone will experience the same progression.
And I think people feel that there has to be a solution, or a pathway.
Editor’s note: This article has been faithfully transcribed from the original interview filmed with the author, and carefully edited and proofread. Edit date: 2026
Discover more about
Solving endometriosis
Mui, B.W.H. et al, 2026, Hyaluronic acid and tissue mechanics orchestrate mammalian digit tip regeneration. Science, Vol 392, Issue 6794.
Raffaelli, A., Wyatt, T.P.J., Simon, C.S., Wenger, L., Niakan, K.K., Ewa K Paluch, E.K.., Chalut, K.L. 2026, Basement membrane mechanics drives patterned response to developmental signalling. bioRxiv 2026.02.13.705301 preprint.
Segel, M., Neumann, B., Hill, M.F.E. et al, 2019, Niche stiffness underlies the ageing of central nervous system progenitor cells. Nature, 573, 130–134.